Tonsil Stones: Discover what they are, how they appear, and how to get rid of them forever. pssss
Tonsil Stones: Discover what they are, how they appear, and how to get rid of them forever.

What Are Tonsil Stones?
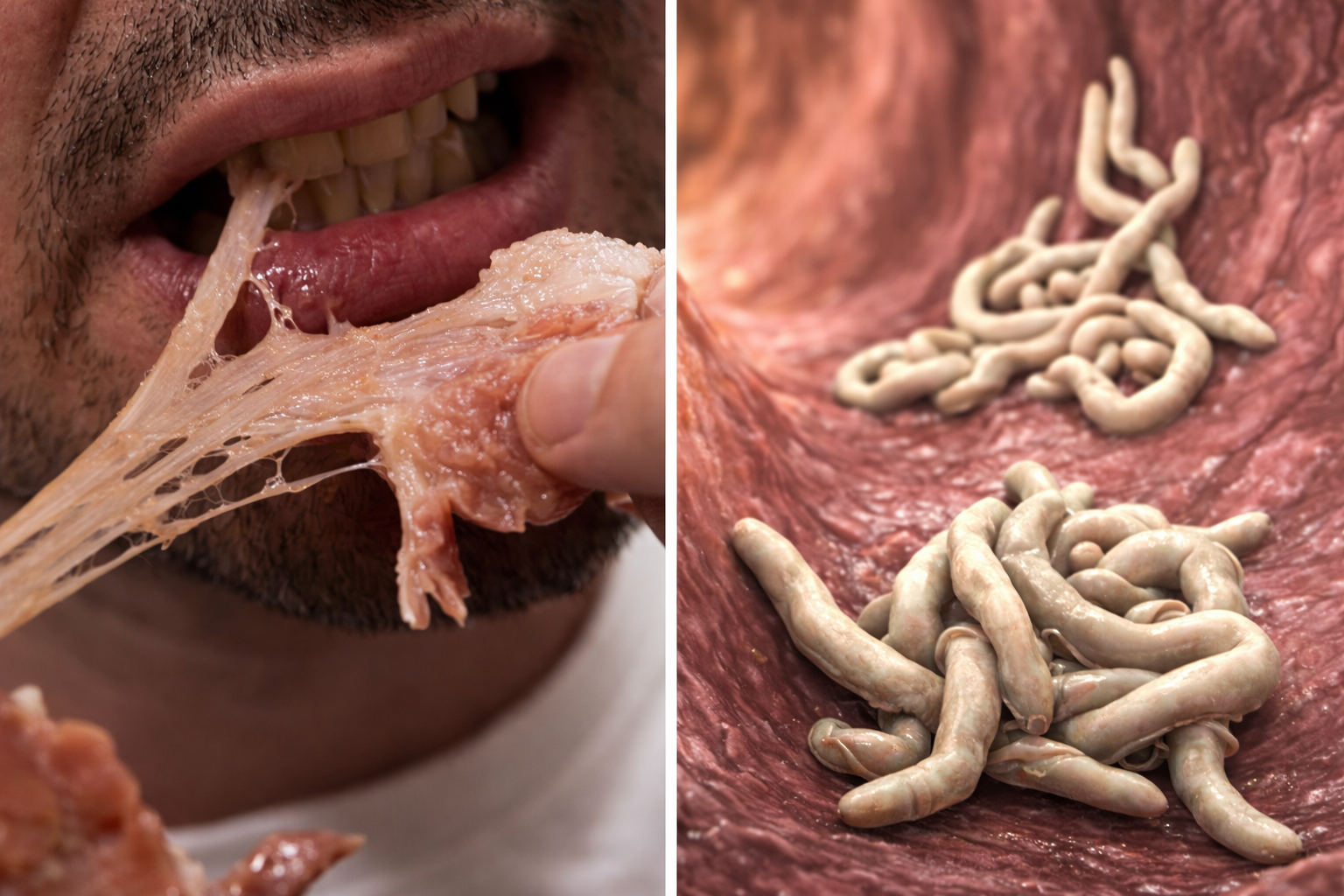
Tonsil stones, also known as tonsilloliths or caseum, are small calcified formations that appear in the tonsils. They consist of food debris, bacteria, and dead cells that, over time, accumulate in the crevices of the tonsils. As these materials build up, they harden and form these small "stones."
While tonsil stones are usually not dangerous, they can cause discomfort in the throat, bad breath, and, in some cases, pain when swallowing. Understanding how they form and how to eliminate them can help you avoid discomfort and maintain good oral health.
How Do Tonsil Stones Form?
Tonsil stones often form when food residues, bacteria, and mucus become trapped in the tonsil crypts (the small crevices or folds in the tonsils). This material hardens over time and turns into stones, or tonsil stones. People with larger tonsils or deeper crevices are more prone to developing these deposits. Additionally, poor oral hygiene, frequent infections, and respiratory issues can increase the risk of tonsil stone formation.
Symptoms Associated with Tonsil Stones
Although tonsil stones do not always cause symptoms, there are some signs that might indicate their presence:
-
Persistent bad breath: Caused by the bacteria that accumulate in the tonsils.
-
Feeling of a foreign object in the throat: This can lead to discomfort when swallowing.
-
Ear pain: Because the tonsils and ears are connected through nerves, ear pain can occur.
-
Inflammation and redness of the tonsils: In more severe cases, tonsils may become swollen and inflamed.
How to Care for Yourself to Prevent Tonsil Stones
To reduce the risk of tonsil stone formation, follow these tips:
-
Maintain good oral hygiene: Brush your teeth after every meal and floss to remove food particles.
-
Regularly use mouthwash: Antibacterial mouthwashes help eliminate bacteria that contribute to tonsil stone formation.
-
Stay hydrated: Drinking water helps keep the mouth and throat clean.
-
Avoid tobacco and alcohol: These substances can irritate the tonsils and promote bacterial accumulation.
How to Safely Remove Tonsil Stones
There are several options for safely removing tonsil stones. Here are some of the most common methods:
-
Gargling with warm salt water: This helps dissolve tonsil stones and reduce inflammation.
-
Using an oral irrigator: Oral irrigators can direct a stream of water to the tonsils to remove deposits without causing harm.
-
Using a cotton swab: With great care, you can gently press the tonsil to extract the tonsil stone.
-
Consult a healthcare professional: If you have large or recurrent tonsil stones, a doctor can remove them and may recommend a tonsillectomy if necessary.
Conclusion
Tonsil stones can be bothersome, but maintaining good oral hygiene and seeking professional help if symptoms persist is crucial for effectively preventing and eliminating them. Remember, while tonsil stones are generally not harmful, early attention can save you from discomfort and improve your overall oral health.
Trusted Sources:
-
Mayo Clinic: Tonsillitis and Tonsil Stones
-
American Dental Association: Oral Hygiene Tips
-
WebMD: How to Treat Tonsil Stones
White Bumps on Mouth: 7 Alarming Causes & Fixes

Seeing white spots or bumps inside your mouth can worry you. But, most of the time, they are not serious and go a way by themselves. It’s important to know why they happen to tell the difference between harmless and serious issues.Found white bumps on mouth? This guide explores 7 alarming causes, from canker sores to oral cancer, and the best, proven fixes.
At Liv Hospital, we use the latest tools and care with kindness. We make sure each patient gets a detailed check-up and advice that fits their needs. For example, canker sores are very common, affecting about 20 percent of people.
We will look into why these oral conditions happen, like canker sores, oral candidiasis, and leukoplakia. We’ll also talk about when you should see a doctor. Knowing the reasons and signs is key to getting the right treatment.
Key Takeaways
- Canker sores are a common cause of white bumps inside the mouth.
- Oral candidiasis and leukoplakia are other possible causes.
- Understanding the causes is key for the right diagnosis and treatment.
- At Liv Hospital, patients get a detailed check-up and care that fits them.
- Seeing a doctor is important for issues that need it.
Understanding Oral Lesions and Their Significance

Oral lesions can be a cause for concern. It’s important to understand their significance for good oral health. White bumps or spots inside the mouth can appear for many reasons. Recognizing their implications is key.
Common Locations for White Spots in the Mouth
White spots or bumps can show up in various places inside the mouth. They often appear on the inside of the cheeks, lips, gums, tongue, and the roof of the mouth. For example, oral lichen planus, a chronic inflammatory condition, can cause white patches or lacy threads on the inside of the cheeks. These spots can be harmless or show a need for attention.
Many people notice small white bumps on the inside of their mouth or tiny white spots on the roof of their mouth. These can be caused by irritation, infection, or other conditions.
Distinguishing Normal Variations from Concerning Signs
It’s important to tell normal variations from signs that need medical attention. While some white bumps may be benign and go away on their own, others can signal a condition that needs treatment. For instance, a white thing in your mouth could be oral thrush, a yeast infection that needs medical care.
We suggest being mindful of any changes in your oral health. If you notice persistent or concerning symptoms, see a healthcare professional. Knowing about oral lesions and their causes can help you keep your mouth healthy.
Common Causes of White Bumps on Mouth

White bumps on the mouth’s mucous membranes can be scary. But knowing what causes them can help. We’ll look at common reasons like canker sores, oral thrush, and irritation from dental appliances or trauma.
Canker Sores: Painful White Lesions with Red Borders
Canker sores are small, painful ulcers that can pop up on the gums, tongue, or inner cheeks. They start as white or yellowish spots with a red border. “These sores are not contagious, but they can be quite painful and uncomfortable.” The exact cause is unknown, but stress, minor injuries, or certain foods can trigger them.
Oral Thrush: Yeast Overgrowth in the Mouth
Oral thrush is caused by too much Candida fungus in the mouth. It shows up as white patches or spots on the tongue, inner cheeks, or roof of the mouth. Oral thrush is more common in infants, older adults, and people with weakened immune systems. It can be triggered by antibiotics, diabetes, and poor oral hygiene.
Irritation from Dental Appliances or Trauma
Irritation from dental appliances, like braces or dentures, can cause white bumps or spots in the mouth. Trauma to the mouth, like biting the inside of the cheek, can also lead to these lesions. Identifying and addressing the source of irritation can help in resolving these bumps. Adjusting or repairing dental appliances can often solve the problem.
Knowing why white bumps appear on the mouth is key to managing them. By figuring out if it’s canker sores, oral thrush, or irritation, you can take the right steps. This helps to ease symptoms and prevent them from coming back.
Canker Sores: The Most Prevalent Oral Lesions
Seeing tiny white spots in your mouth can be scary, but they’re often just canker sores. These are small, shallow lesions that pop up on soft mouth tissues. They can hurt and make it hard to eat, drink, or even talk.
Appearance and Symptoms
Canker sores look like small, round or oval white or yellowish lesions with a red edge. They can show up anywhere in your mouth, like on your lips, cheeks, tongue, or gums. You might feel a burning or tingling before they appear, followed by pain or discomfort when eating or drinking.
There are three types of canker sores: minor, major, and herpetiform. Minor sores are small and heal in a week or two. Major sores are bigger and hurt more, taking longer to heal. Herpetiform sores are a cluster of small sores.
Common Triggers
Knowing what causes canker sores can help prevent them. Common causes include stress, certain foods like citrus or spicy ones, and mouth injuries. Hormonal changes, nutritional deficiencies, or some medications can also cause them.
To deal with canker sores, it’s key to know and avoid triggers. Keeping your mouth clean and avoiding irritating foods can help prevent them.
Typical Healing Timeline
Most canker sores heal on their own in one to three weeks without scarring. Using numbing creams or gels can ease the pain. For severe or lasting sores, your doctor might suggest prescription meds or dental lasers.
Understanding canker sores helps manage them better. Knowing their look, symptoms, causes, and healing time can reduce discomfort. If you get canker sores often or they’re really bad, see a healthcare pro for advice.
Oral Candidiasis: When Yeast Causes White Patches
When yeast grows too much in the mouth, it can cause oral candidiasis. This condition is also known as thrush. It shows up as white, creamy patches on the tongue, inner cheeks, or roof of the mouth. These patches can be wiped off, revealing red, inflamed areas underneath.
Identifying Thrush in Different Age Groups
Oral candidiasis can affect people of all ages. In infants, it can make feeding uncomfortable. In adults, it might be linked to health issues or certain medicines.
- Infants: Thrush shows up as white patches on the tongue or inside the cheeks, often with diaper rash.
- Adults: Oral candidiasis presents with white patches that can hurt, making eating or drinking painful.
- Elderly: Older adults are more likely to get oral candidiasis due to denture use or less saliva.
Risk Factors: Antibiotics, Immune Suppression, and Diabetes
Several factors can raise the risk of oral candidiasis. These include:
- Antibiotics: Broad-spectrum antibiotics can upset the mouth’s normal balance, letting Candida grow too much.
- Immune Suppression: People with weakened immune systems, like those with HIV/AIDS or on chemotherapy, are more at risk.
- Diabetes: High blood sugar helps Candida grow, raising the risk of oral candidiasis.
- Denture Use: Poorly fitting dentures or not cleaning them well can lead to thrush.
Treatment Approaches for Oral Candidiasis
Treatment for oral candidiasis usually involves antifungal medications. The treatment depends on how severe it is and the patient’s health.
- Topical Treatments: Antifungal gels or liquids, like Nystatin, are applied directly to the affected areas.
- Systemic Treatments: In severe cases or for those with weakened immune systems, oral antifungal medicines are used.
- Good Oral Hygiene: Keeping good oral hygiene, like regular brushing and flossing, can help prevent it from coming back.
Understanding the causes, risk factors, and treatments for oral candidiasis helps us manage it better. This way, we can prevent its complications.
Leukoplakia: Potentially Serious White Patches
Leukoplakia is a condition with thick, white patches that can’t be wiped away. These patches can show up anywhere in the mouth. They are linked to a higher risk of oral cancer. Knowing about leukoplakia helps catch it early and prevent serious problems.
Distinguishing Features
Leukoplakia is different from other white mouth lesions because it doesn’t go away. It sticks to the mucous membranes, unlike oral thrush. It’s important to tell leukoplakia apart from canker sores or oral lichen planus because treatment and risks are different.
Leukoplakia looks like white or gray patches that can be flat or slightly raised. These patches can be on the tongue, floor of the mouth, or other parts of the mouth. The texture can be smooth, rough, or corrugated.
Risk Factors and Causes
Leukoplakia often comes from using tobacco products, like smoking or smokeless tobacco. Drinking alcohol also raises the risk. Long-term irritation from rough teeth, dental appliances, or other things can also cause leukoplakia.
“The use of tobacco products is the most significant risk factor for developing leukoplakia, highlighting the importance of tobacco cessation in preventing oral potentially malignant disorders.”
Monitoring and Management
Because leukoplakia can turn into oral cancer, it’s important to watch it closely. This might mean regular check-ups with a healthcare provider and sometimes a biopsy. Treatment can include stopping the cause of irritation, quitting tobacco and alcohol, and sometimes removing the lesion surgically.
Early detection and proper treatment of leukoplakia are key to stopping it from getting worse. Regular dental visits and staying aware of changes in your mouth are important for managing this condition.
Oral Lichen Planus and Autoimmune Conditions
Many patients come to us with oral lichen planus. This condition shows up as white, lacy patches or red, inflamed tissues in the mouth. It’s an immune-mediated inflammatory condition that can cause a lot of discomfort and needs careful management.
Recognizing the Lacy Pattern of Lichen Planus
Oral lichen planus is known for its distinctive lacy pattern. It often shows up as white, thread-like lesions or patches inside the cheeks. This unique appearance helps us diagnose the condition.
The lacy pattern comes from the immune system’s response. This leads to inflammation and the formation of these lesions. It’s important to recognize this pattern to tell oral lichen planus apart from other conditions that cause little white bumps inside the mouth or white spots in the mouth.
Associated Symptoms and Discomfort
Patients with oral lichen planus often feel pain, burning sensations, and discomfort. This is worse when they eat spicy or acidic foods. The condition can also cause red, inflamed areas, in addition to the white lacy patches.
“The presence of oral lichen planus can significantly impact a patient’s quality of life, necessitating a thorough treatment plan to manage symptoms and prevent complications.”
In some cases, oral lichen planus is linked to other autoimmune conditions. It’s important to watch for signs of these related conditions.
Long-term Management Strategies
Managing oral lichen planus needs a long-term approach. We focus on reducing symptoms, preventing flare-ups, and watching for any complications, like oral cancer. Regular visits to a periodontist or oral medicine specialist are key.
|
Management Strategy |
Description |
|
Topical Corticosteroids |
Used to reduce inflammation and manage symptoms |
|
Antihistamines |
Can help alleviate discomfort and itching |
|
Regular Monitoring |
Essential for early detection of complications |
With a thorough management plan, patients with oral lichen planus can control their symptoms better. This reduces the risk of complications.
Less Common Causes of White Oral Spots
Many conditions can cause white bumps or spots inside the mouth, aside from the usual ones. Knowing about these can help people understand and manage their symptoms better.
Fordyce Spots: Harmless Oil Glands
Fordyce spots are small, harmless oil glands. They look like white or yellowish bumps on the lips, inside the cheeks, or genital area. They are usually painless and don’t need treatment. These spots are quite common and are seen as a normal part of our anatomy.
Mucoceles and Oral Fibromas
Mucoceles are mucus-filled cysts that look like white or translucent bumps in the mouth. They often happen after minor trauma. Oral fibromas are benign growths that look like white or pink bumps. They usually happen because of irritation. Both are generally harmless but can be removed if they cause discomfort.
- Mucoceles often occur on the lower lip.
- Oral fibromas can appear anywhere in the mouth.
- Both are typically painless but can be bothersome.
Linea Alba: The White Line on Your Cheek
Linea alba, or “white line” in Latin, is a condition with a white line or ridge on the inside of the cheek. It happens because of chronic irritation or friction. It’s considered harmless.
Some key points about linea alba include:
- It is often associated with teeth grinding or clenching.
- The condition is more common in individuals with a high occlusal plane.
- No treatment is necessary, but addressing the underlying cause of friction can help alleviate the condition.
By understanding these less common causes of white oral spots, individuals can better identify their condition. They can then seek the right advice or treatment if needed.
When to See a Healthcare Provider
Many white bumps in the mouth are harmless. But, some signs mean you should see a doctor. Knowing these signs helps you get help when you need it.
Warning Signs That Require Professional Evaluation
Some white bumps or spots in the mouth need a doctor’s check. Look out for these signs:
- White spots that don’t go away after two weeks
- Spots that bleed, thicken, or become painful
- Recurring or worsening sores
- Difficulty swallowing or pain while swallowing
- Presence of fever or other systemic symptoms
If you notice any of these, see a doctor. They can find out what’s wrong and how to fix it.
What to Expect During Diagnosis
When you see a doctor for white bumps or spots, they’ll check you thoroughly. This might include:
- A visual inspection of your mouth, tongue, and throat
- A review of your medical history to identify possible causes
- Questions about your symptoms, including when they started and any factors that make them better or worse
The doctor might also do more tests to find out why you have white bumps.
Possible Tests and Procedures
Based on what they find, the doctor might suggest more tests or procedures. These could be:
- A biopsy to examine a tissue sample under a microscope
- Cultures to check for fungal or bacterial infections
- Blood tests to assess your overall health and identify possible underlying conditions
Knowing why you have white bumps or spots is key to treating them right. By getting a professional check-up when needed, you can fix oral health problems fast and well.
Conclusion: Prevention and Management of Oral White Bumps
To prevent and manage oral white bumps, we need a complete plan. Keeping your mouth clean is key. Also, avoid things like tobacco and too much alcohol. Managing stress helps too, to avoid problems like canker sores and leukoplakia.
Knowing why mouth small white bumps happen helps us act early. Tiny white spots in your mouth might mean something’s off. White bumps inside could mean you need to see a doctor.
Regular dental visits and a healthy diet are important. These habits help keep your mouth healthy. Knowing what causes oral white bumps helps you avoid them.
Managing oral white bumps means good oral care and staying away from irritants. If you have persistent or worrying lesions, see a doctor. We suggest talking to a healthcare provider if you have concerns.
FAQ
What are the common causes of white bumps inside the mouth?
White bumps inside the mouth can come from different things. Canker sores, oral candidiasis, leukoplakia, and irritation from dental appliances or trauma are common causes.
How can I differentiate between harmless white spots and signs of a more serious condition?
Harmless white spots are usually small and don’t hurt. But, serious conditions might hurt, be red, or make it hard to swallow. If you’re not sure, it’s best to see a healthcare provider.
What are canker sores, and how can they be managed?
Canker sores are painful white spots with red edges. They can be caused by stress, certain foods, or minor injuries. They usually heal in a week or two. To manage them, avoid triggers and use topical treatments to ease pain.
What is oral candidiasis, and how is it treated?
Oral candidiasis, or thrush, is a yeast overgrowth in the mouth. It causes white patches. Treatment includes antifungal medications. It’s important to address risk factors like antibiotics, immune suppression, and diabetes.
What is leukoplakia, and why is it a concern?
Leukoplakia is a condition with white patches in the mouth. It can be precancerous. It’s linked to tobacco, alcohol, and chronic irritation. It’s important to monitor and manage its precancerous risk.
When should I seek professional help for white bumps in my mouth?
See a healthcare provider if you have persistent or severe symptoms. This includes pain, difficulty swallowing, or if you’re unsure about the cause. They can give a proper diagnosis and treatment.
What can I expect during a diagnosis for white bumps in my mouth?
During a diagnosis, a healthcare provider will examine your mouth and review your medical history. They may also do tests or procedures to find the cause of the white bumps.
May you like
How can I prevent white bumps from occurring in my mouth?
To prevent white bumps, keep good oral hygiene. Avoid triggers like certain foods or tobacco. Also, manage conditions like diabetes or immune suppression.
References
National Center for Biotechnology Information. Oral Mucosal Lesions: Prevalence, Types, Etiology, and Management. Retrieved from