Doctors Alert: Why Some Popular Foods May Carry Parasite Risks News
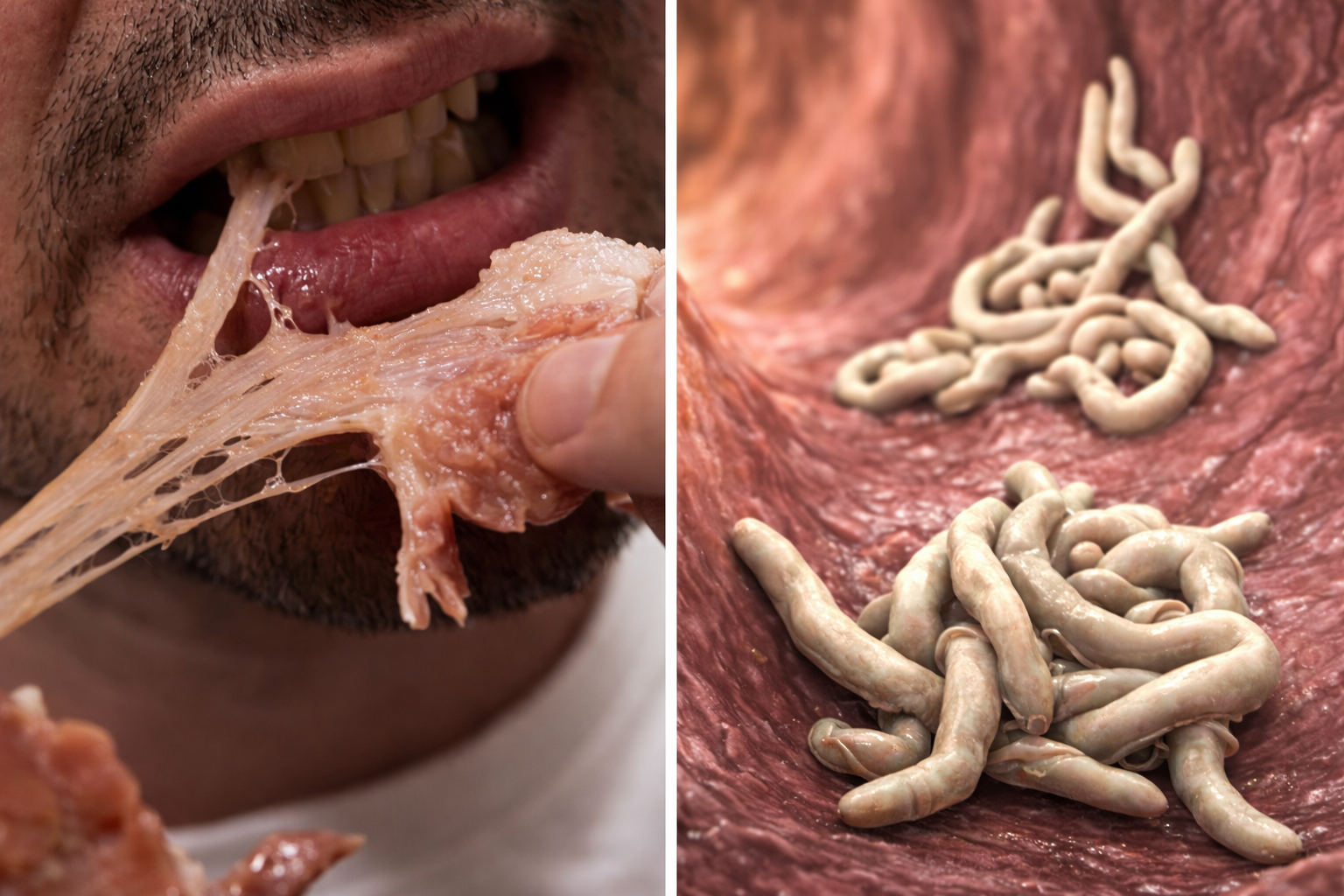
A striking image circulating online shows a raw seafood item opened up, with red circles highlighting what appear to be worm-like organisms. Paired with the warning, “Doctors Alert: Stop Eating These Four Foods Right Away; They’re Often Linked to Parasites,” the post has sparked anxiety—and many questions—about which foods may contain parasites and how to stay safe.
While the headline is dramatic, the underlying issue is real: parasites can be found in certain foods, especially when they are eaten raw or undercooked. The good news is that safe handling, proper cooking, and trusted sourcing can greatly reduce the risk.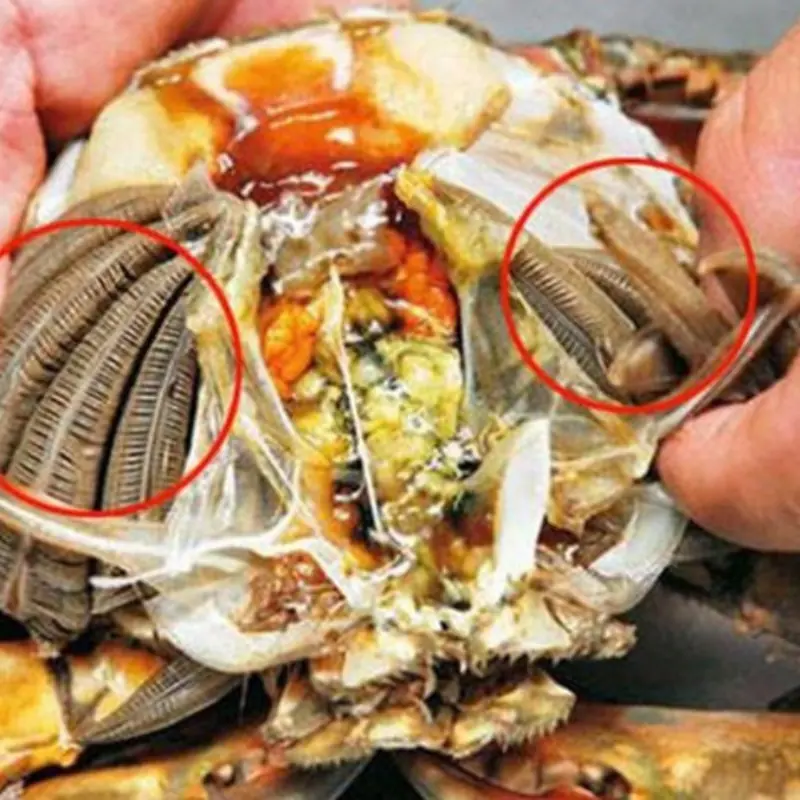
What the Image Suggests
The photo appears to show seafood with visible parasite-like strands. In many cases, these may be nematodes (roundworms) or other organisms found in marine animals. Parasites occur naturally in ocean ecosystems, and fish or shellfish can become hosts during their life cycle.
However, an image alone cannot confirm the exact species. What it does highlight is an important point: food can look normal and still contain parasites, and sometimes parasites can be visible if the product is heavily infested.
The Four Foods Most Often Linked to Parasites
Health experts commonly warn that parasites are more likely in certain types of foods—particularly those eaten raw, lightly cooked, or improperly processed.
1) Raw or Undercooked Seafood
Sushi, sashimi, raw oysters, and lightly cooked squid or crab are popular in many cultures. But raw seafood carries a higher risk of parasites such as anisakis. Symptoms can include stomach pain, nausea, vomiting, and allergic reactions.
Safer choice: Eat seafood fully cooked, or choose reputable restaurants that follow strict freezing standards for raw fish.
2) Raw or Undercooked Freshwater Fish
Freshwater fish can host parasites that affect the liver or intestines. In some regions, dishes made with raw freshwater fish have been linked to serious infections.
Safer choice: Cook freshwater fish thoroughly and avoid raw freshwater dishes unless they meet verified safety standards.
3) Undercooked Pork
Pork is associated with parasites such as tapeworms and, in rare cases, trichinella (depending on farming and food safety controls). Most modern pork is safer than in the past, but undercooking still increases risk.
Safer choice: Cook pork to a safe internal temperature and avoid tasting meat before it is fully cooked.
4) Unwashed Produce (Especially Leafy Greens)
Parasites are not only in meat and fish. Fruits and vegetables can be contaminated through soil, untreated water, or handling. Leafy greens and herbs are common culprits because they are eaten raw and can trap dirt.
Safer choice: Wash produce well, soak when appropriate, and buy from trusted sources.
Signs of Possible Parasite Infection
People may experience different symptoms depending on the parasite and the immune system. Common warning signs can include:
-
Persistent stomach pain or cramps
-
Nausea and vomiting
-
Diarrhea
-
Unexplained weight loss
-
Fatigue
-
Itching or rashes (sometimes allergic-type reactions)
If symptoms appear after eating raw or suspicious food, seek medical advice—especially if symptoms are severe or last more than a day or two.
How to Protect Yourself: Simple Food Safety Steps
The most effective protection is not fear—it’s prevention.
Cook Thoroughly
Heating food properly kills most parasites. This is especially important for seafood, pork, and freshwater fish.
Freeze When Needed
Many parasites in fish are killed by proper freezing. Reputable restaurants and suppliers typically follow freezing guidelines for fish served raw.
Buy From Trusted Sellers
Choose suppliers with good hygiene and quality control. Avoid seafood that smells unusual, looks slimy, or comes from unclear sources.
Clean Your Kitchen
Wash hands, boards, and knives after handling raw meat or seafood, and keep raw foods separate from ready-to-eat items.
Bottom Line: Don’t Panic—Be Smart
The viral message may be exaggerated, but the risk is real in certain situations. Parasites are part of nature, especially in marine and freshwater environments. Instead of avoiding entire food groups forever, focus on safe sourcing, proper cooking, and good hygiene.
Food can still be delicious and safe—when prepared correctly.
Doctors Alert: Stop Eating These Foods Right Away pssss
Doctors Alert: Stop Eating These Foods Right Away

𝟸 𝚍𝚎𝚊𝚍 𝚊𝚏𝚝𝚎𝚛 𝚎𝚊𝚝𝚒𝚗𝚐 𝚘𝚢𝚜𝚝𝚎𝚛𝚜, 𝚌𝚘𝚗𝚝𝚛𝚊𝚌𝚝𝚒𝚗𝚐 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊, 𝚘𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚜𝚊𝚢
𝚃𝚠𝚘 𝚙𝚎𝚘𝚙𝚕𝚎 𝚊𝚛𝚎 𝚍𝚎𝚊𝚍 𝚊𝚏𝚝𝚎𝚛 𝚎𝚊𝚝𝚒𝚗𝚐 𝚛𝚊𝚠 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚊𝚗𝚍 𝚌𝚘𝚗𝚝𝚛𝚊𝚌𝚝𝚒𝚗𝚐 𝚊 𝚍𝚎𝚊𝚍𝚕𝚢 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊, 𝚊𝚌𝚌𝚘𝚛𝚍𝚒𝚗𝚐 𝚝𝚘 𝚘𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜.
𝚃𝚑𝚎 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝙸𝚕𝚕𝚞𝚖𝚒𝚗𝚊𝚝𝚘𝚛 𝚛𝚎𝚙𝚘𝚛𝚝𝚜 𝚝𝚑𝚊𝚝 𝚝𝚑𝚎 𝚍𝚎𝚊𝚝𝚑𝚜 𝚠𝚎𝚛𝚎 𝚌𝚊𝚞𝚜𝚎𝚍 𝚋𝚢 𝚝𝚑𝚎 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊, 𝚅𝚒𝚋𝚛𝚒𝚘 𝚟𝚞𝚕𝚗𝚒𝚏𝚒𝚌𝚞𝚜, 𝚠𝚑𝚒𝚌𝚑 𝚑𝚞𝚖𝚊𝚗𝚜 𝚌𝚊𝚗 𝚐𝚎𝚝 𝚏𝚛𝚘𝚖 𝚎𝚊𝚝𝚒𝚗𝚐 𝚛𝚊𝚠 𝚜𝚎𝚊𝚏𝚘𝚘𝚍.
𝙷𝚞𝚖𝚊𝚗𝚜 𝚌𝚊𝚗 𝚊𝚕𝚜𝚘 𝚐𝚎𝚝 𝚝𝚑𝚎 𝚒𝚗𝚏𝚎𝚌𝚝𝚒𝚘𝚗 𝚏𝚛𝚘𝚖 𝚐𝚘𝚒𝚗𝚐 𝚒𝚗𝚝𝚘 𝚋𝚘𝚍𝚒𝚎𝚜 𝚘𝚏 𝚠𝚊𝚝𝚎𝚛 𝚠𝚑𝚒𝚕𝚎 𝚑𝚊𝚟𝚒𝚗𝚐 𝚊𝚗 𝚘𝚙𝚎𝚗 𝚠𝚘𝚞𝚗𝚍.
𝙾𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚠𝚒𝚝𝚑 𝚝𝚑𝚎 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝙳𝚎𝚙𝚊𝚛𝚝𝚖𝚎𝚗𝚝 𝚘𝚏 𝙷𝚎𝚊𝚕𝚝𝚑 𝚜𝚊𝚒𝚍 𝚝𝚑𝚎 𝚝𝚠𝚘 𝚍𝚎𝚊𝚝𝚑𝚜 𝚊𝚛𝚎 𝚊𝚝𝚝𝚛𝚒𝚋𝚞𝚝𝚎𝚍 𝚝𝚘 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚝𝚑𝚊𝚝 𝚠𝚎𝚛𝚎 𝚑𝚊𝚛𝚟𝚎𝚜𝚝𝚎𝚍 𝚒𝚗 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊.
𝚃𝚑𝚎 𝚝𝚠𝚘 𝚙𝚎𝚘𝚙𝚕𝚎 𝚊𝚝𝚎 𝚝𝚑𝚎 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚊𝚝 𝚝𝚠𝚘 𝚜𝚎𝚙𝚊𝚛𝚊𝚝𝚎 𝚛𝚎𝚜𝚝𝚊𝚞𝚛𝚊𝚗𝚝𝚜, 𝚘𝚗𝚎 𝚒𝚗 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝚊𝚗𝚍 𝚝𝚑𝚎 𝚘𝚝𝚑𝚎𝚛 𝚒𝚗 𝙵𝚕𝚘𝚛𝚒𝚍𝚊. 𝙾𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚍𝚒𝚍 𝚗𝚘𝚝 𝚙𝚛𝚘𝚟𝚒𝚍𝚎 𝚝𝚑𝚎 𝚗𝚊𝚖𝚎𝚜 𝚘𝚏 𝚝𝚑𝚎 𝚛𝚎𝚜𝚝𝚊𝚞𝚛𝚊𝚗𝚝𝚜.
𝚂𝚝𝚊𝚝𝚎 𝚘𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚒𝚗 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝚜𝚊𝚒𝚍 𝚝𝚑𝚎𝚛𝚎 𝚊𝚛𝚎 𝚗𝚘𝚠 𝚜𝚒𝚡 𝚝𝚘𝚝𝚊𝚕 𝚍𝚎𝚊𝚝𝚑𝚜 𝚏𝚛𝚘𝚖 𝚅𝚒𝚋𝚛𝚒𝚘 𝚟𝚞𝚕𝚗𝚒𝚏𝚒𝚌𝚞𝚜 𝚕𝚒𝚗𝚔𝚎𝚍 𝚝𝚘 𝚝𝚑𝚎 𝚜𝚝𝚊𝚝𝚎. 𝙸𝚝 𝚒𝚜 𝚞𝚗𝚌𝚕𝚎𝚊𝚛 𝚒𝚏 𝚝𝚑𝚎 𝚘𝚝𝚑𝚎𝚛 𝚏𝚘𝚞𝚛 𝚍𝚎𝚊𝚝𝚑𝚜 𝚠𝚎𝚛𝚎 𝚌𝚊𝚞𝚜𝚎𝚍 𝚋𝚢 𝚎𝚊𝚝𝚒𝚗𝚐 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚘𝚛 𝚏𝚛𝚘𝚖 𝚘𝚙𝚎𝚗 𝚠𝚘𝚞𝚗𝚍𝚜 𝚒𝚗 𝚠𝚊𝚝𝚎𝚛.
𝙲𝚊𝚜𝚎𝚜 𝚘𝚏 𝚝𝚑𝚎 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊 𝚊𝚛𝚎 𝚘𝚗 𝚝𝚑𝚎 𝚛𝚒𝚜𝚎.
𝙰𝚌𝚌𝚘𝚛𝚍𝚒𝚗𝚐 𝚝𝚘 𝚝𝚑𝚎 𝙲𝙳𝙲, 𝚝𝚑𝚎 𝚙𝚘𝚝𝚎𝚗𝚝𝚒𝚊𝚕𝚕𝚢 𝚍𝚎𝚊𝚍𝚕𝚢 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊 𝚝𝚑𝚛𝚒𝚟𝚎 𝚒𝚗 𝚌𝚘𝚊𝚜𝚝𝚊𝚕 𝚠𝚊𝚝𝚎𝚛𝚜 𝚍𝚞𝚛𝚒𝚗𝚐 𝚠𝚊𝚛𝚖𝚎𝚛 𝚖𝚘𝚗𝚝𝚑𝚜, 𝚎𝚜𝚙𝚎𝚌𝚒𝚊𝚕𝚕𝚢 𝚒𝚗 𝚋𝚛𝚊𝚌𝚔𝚒𝚜𝚑 𝚠𝚊𝚝𝚎𝚛𝚜, 𝚠𝚑𝚎𝚛𝚎 𝚏𝚛𝚎𝚜𝚑 𝚠𝚊𝚝𝚎𝚛 𝚖𝚎𝚎𝚝𝚜 𝚝𝚑𝚎 𝚜𝚎𝚊.
𝙲𝚊𝚜𝚎𝚜 𝚘𝚏 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊 𝚠𝚎𝚛𝚎 𝚘𝚗𝚌𝚎 𝚕𝚊𝚛𝚐𝚎𝚕𝚢 𝚌𝚘𝚗𝚏𝚒𝚗𝚎𝚍 𝚝𝚘 𝚝𝚑𝚎 𝙶𝚞𝚕𝚏 𝙲𝚘𝚊𝚜𝚝, 𝚋𝚞𝚝 𝚝𝚑𝚎 𝙲𝙳𝙲 𝚜𝚊𝚒𝚍 𝚌𝚊𝚜𝚎𝚜 𝚏𝚛𝚘𝚖 𝟷𝟿𝟾𝟾 𝚝𝚘 𝟸0𝟷𝟾 𝚜𝚞𝚛𝚐𝚎𝚍 𝚊𝚕𝚘𝚗𝚐 𝚝𝚑𝚎 𝙴𝚊𝚜𝚝 𝙲𝚘𝚊𝚜𝚝 𝚠𝚒𝚝𝚑 𝚊𝚗 𝟾00% 𝚒𝚗𝚌𝚛𝚎𝚊𝚜𝚎.
𝚃𝚑𝚎 𝚛𝚒𝚜𝚔 𝚏𝚘𝚛 𝚅𝚒𝚋𝚛𝚒𝚘 𝚒𝚗𝚏𝚎𝚌𝚝𝚒𝚘𝚗𝚜 𝚑𝚊𝚜 𝚊𝚕𝚜𝚘 𝚜𝚙𝚛𝚎𝚊𝚍 𝚏𝚊𝚛𝚝𝚑𝚎𝚛 𝚗𝚘𝚛𝚝𝚑 𝚊𝚜 𝚠𝚊𝚝𝚎𝚛 𝚝𝚎𝚖𝚙𝚎𝚛𝚊𝚝𝚞𝚛𝚎𝚜 𝚑𝚊𝚟𝚎 𝚒𝚗𝚌𝚛𝚎𝚊𝚜𝚎𝚍 𝚍𝚞𝚎 𝚝𝚘 𝚌𝚕𝚒𝚖𝚊𝚝𝚎 𝚌𝚑𝚊𝚗𝚐𝚎.
𝙰𝚌𝚌𝚘𝚛𝚍𝚒𝚗𝚐 𝚝𝚘 𝚝𝚑𝚎 𝙲𝙳𝙲, 𝚊𝚋𝚘𝚞𝚝 𝟷 𝚒𝚗 𝟻 𝚙𝚎𝚘𝚙𝚕𝚎 𝚠𝚒𝚝𝚑 𝚝𝚑𝚎 𝚒𝚗𝚏𝚎𝚌𝚝𝚒𝚘𝚗 𝚍𝚒𝚎.
Contaminated oysters spread fatal flesh-eating bacteria in two states
Two latest deaths were traced back to Louisiana-harvested oysters
Two people have died after eating oysters contaminated with flesh-eating bacteria, health officials confirmed, and others have been infected.
Both of the fatal cases were traced to Louisiana-harvested oysters that ended up on plates in restaurants in Louisiana and Florida.
The bacterium, Vibrio vulnificus, has now been linked to six deaths in Louisiana and five deaths in Florida, according to the states' health departments.
The rising number of outbreaks prompted the Louisiana Department of Health to issue a statement July 31, urging residents to take precautions against vibriosis, the infection caused by Vibrio vulnificus.
Vibrio vulnificus is part of a wider group of Vibrio bacteria, which are found in coastal waters, the Centers for Disease Control and Prevention states.

Most people get vibriosis by eating raw or undercooked shellfish, particularly oysters, according to the CDC. In some cases, it can also enter open wounds while people are swimming. (iStock)
Vibrio has the potential to cause severe infections, according to Dr. Andrew Handel, pediatric infectious diseases specialist at Stony Brook Children's Hospital in New York.
These include invasive soft tissue infections (sometimes called "necrotizing fasciitis" or "flesh-eating bacteria") and bloodstream infections.
Most people get vibriosis by eating raw or undercooked shellfish, particularly oysters, according to the CDC.
In some cases, it can also enter open wounds while people are swimming.

People who have eaten contaminated shellfish will have severe vomiting and diarrhea, which can lead to dehydration, health officials caution. (iStock)
Prior to this incident, health officials reported 17 cases of Vibrio vulnificus among Louisiana residents in 2025. All patients were hospitalized, and four of those illnesses resulted in death.
Over the previous 10 years, an average of seven Vibrio vulnificus cases and one death were reported each year in Louisiana.
"It’s just prolific right now," Jennifer Armentor, the molluscan shellfish program administrator at the Louisiana Department of Health, told the Louisiana Oyster Task Force Tuesday at the New Orleans Lakefront Airport.
Symptoms to watch for
Vibriosis symptoms depend on the type of infection, according to Handel.
"The symptoms of skin infections can progress quickly and become life-threatening in a short time," he previously told Fox News Digital. "Thankfully, those infections are rare."
"If you do eat shellfish, make sure it has not been sitting out for a long time and comes from a hygienic source."
People who have eaten contaminated shellfish will have severe vomiting and diarrhea, which can lead to dehydration, the doctor warned.
While healthy people generally experience only mild symptoms, those who are immunocompromised or have chronic liver disease can face serious health risks.

A bacterial infection is diagnosed by testing cultures obtained from stool, wounds or blood. (iStock)
If Vibrio vulnificus enters the bloodstream, it can cause severe illness marked by fever, chills, septic shock and blistering skin lesions, according to Florida Health. About half of these bloodstream infections are fatal.
Some severe cases can cause necrotizing fasciitis, which is when the flesh around an open wound dies, the CDC cautions.
Diagnosis and treatment
The bacterial infection is diagnosed by testing cultures obtained from stool, wounds or blood, according to health officials.
For mild infections, the CDC recommends increasing fluid intake to prevent dehydration.

About one in five people will die from a vibriosis infection, sometimes within a day or two of the illness. (iStock)
Those with severe or prolonged infections should receive antibiotics to improve survival rates. For people with infected wounds, surgery may be necessary to remove dead tissue.
About one in five people will die from the infection, sometimes within a day or two of the illness, the CDC states.
"To prevent Vibrio food poisoning, avoid eating raw shellfish, especially if you are immunocompromised or have chronic liver disease," Handel advised.
The doctor noted that Vibrio infections are rare and "should not be a major cause of alarm."
"If you do eat shellfish, make sure it has not been sitting out for a long time and comes from a hygienic source."
Fox News Digital's Melissa Rudy contributed reporting.
Khloe Quill is a lifestyle production assistant with Fox News Digital. She and the lifestyle team cover a range of story topics including food and drink, travel, and health.
How to Eat Oysters Safely: Important Tips to Protect Your Health
Oysters are a popular seafood enjoyed around the world for their unique taste and nutritional value. However, eating oysters improperly — especially raw oysters — can pose serious health risks. Health experts emphasize that following proper safety guidelines is essential to avoid foodborne illnesses.
Understand the Risks of Raw Oysters
Raw or undercooked oysters may contain harmful bacteria such as Vibrio, which naturally live in warm coastal waters. These bacteria are invisible, odorless, and cannot be detected by taste.
In some cases, infections can become severe and even life-threatening, particularly for people with weakened immune systems.
Choose Oysters from Reliable Sources
Buy oysters only from licensed and reputable suppliers
Avoid oysters harvested from unregulated or unknown waters
Check that oysters are properly refrigerated and stored
Restaurants and seafood markets should follow strict food safety regulations to reduce contamination risks.
Cook Oysters Thoroughly
Cooking is the most effective way to kill harmful bacteria. Health authorities recommend:
Boiling oysters until shells open and continuing to boil for at least 3–5 minutes
Steaming oysters for 4–9 minutes
Frying, baking, or grilling oysters until the flesh is firm and fully cooked
Avoid eating oysters that do not open during cooking.
Be Extra Careful if You Are High-Risk
The following groups should avoid raw oysters completely:
People with liver disease
Individuals with weakened immune systems
Pregnant women
Older adults
For these individuals, even a small amount of contaminated seafood can cause serious illness.
Practice Good Food Hygiene
Wash hands thoroughly before and after handling raw seafood
Keep raw oysters separate from other foods
Clean knives, cutting boards, and surfaces after use
Proper hygiene helps prevent cross-contamination.
Know the Warning Signs
Seek medical attention immediately if you experience symptoms such as:
Fever
Vomiting or diarrhea
Severe stomach pain
Skin wounds that become red, swollen, or painful after seawater exposure
Early treatment can be life-saving.
Conclusion
Oysters can be enjoyed safely when handled and prepared correctly. Choosing reliable sources, cooking oysters thoroughly, and understanding personal health risks are key steps to protecting yourself and your family.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice.
Doctors Alert: Stop Eating These Foods Right Away
𝟸 𝚍𝚎𝚊𝚍 𝚊𝚏𝚝𝚎𝚛 𝚎𝚊𝚝𝚒𝚗𝚐 𝚘𝚢𝚜𝚝𝚎𝚛𝚜, 𝚌𝚘𝚗𝚝𝚛𝚊𝚌𝚝𝚒𝚗𝚐 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊, 𝚘𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚜𝚊𝚢
𝚃𝚠𝚘 𝚙𝚎𝚘𝚙𝚕𝚎 𝚊𝚛𝚎 𝚍𝚎𝚊𝚍 𝚊𝚏𝚝𝚎𝚛 𝚎𝚊𝚝𝚒𝚗𝚐 𝚛𝚊𝚠 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚊𝚗𝚍 𝚌𝚘𝚗𝚝𝚛𝚊𝚌𝚝𝚒𝚗𝚐 𝚊 𝚍𝚎𝚊𝚍𝚕𝚢 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊, 𝚊𝚌𝚌𝚘𝚛𝚍𝚒𝚗𝚐 𝚝𝚘 𝚘𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜.
𝚃𝚑𝚎 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝙸𝚕𝚕𝚞𝚖𝚒𝚗𝚊𝚝𝚘𝚛 𝚛𝚎𝚙𝚘𝚛𝚝𝚜 𝚝𝚑𝚊𝚝 𝚝𝚑𝚎 𝚍𝚎𝚊𝚝𝚑𝚜 𝚠𝚎𝚛𝚎 𝚌𝚊𝚞𝚜𝚎𝚍 𝚋𝚢 𝚝𝚑𝚎 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊, 𝚅𝚒𝚋𝚛𝚒𝚘 𝚟𝚞𝚕𝚗𝚒𝚏𝚒𝚌𝚞𝚜, 𝚠𝚑𝚒𝚌𝚑 𝚑𝚞𝚖𝚊𝚗𝚜 𝚌𝚊𝚗 𝚐𝚎𝚝 𝚏𝚛𝚘𝚖 𝚎𝚊𝚝𝚒𝚗𝚐 𝚛𝚊𝚠 𝚜𝚎𝚊𝚏𝚘𝚘𝚍.
𝙷𝚞𝚖𝚊𝚗𝚜 𝚌𝚊𝚗 𝚊𝚕𝚜𝚘 𝚐𝚎𝚝 𝚝𝚑𝚎 𝚒𝚗𝚏𝚎𝚌𝚝𝚒𝚘𝚗 𝚏𝚛𝚘𝚖 𝚐𝚘𝚒𝚗𝚐 𝚒𝚗𝚝𝚘 𝚋𝚘𝚍𝚒𝚎𝚜 𝚘𝚏 𝚠𝚊𝚝𝚎𝚛 𝚠𝚑𝚒𝚕𝚎 𝚑𝚊𝚟𝚒𝚗𝚐 𝚊𝚗 𝚘𝚙𝚎𝚗 𝚠𝚘𝚞𝚗𝚍.
𝙾𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚠𝚒𝚝𝚑 𝚝𝚑𝚎 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝙳𝚎𝚙𝚊𝚛𝚝𝚖𝚎𝚗𝚝 𝚘𝚏 𝙷𝚎𝚊𝚕𝚝𝚑 𝚜𝚊𝚒𝚍 𝚝𝚑𝚎 𝚝𝚠𝚘 𝚍𝚎𝚊𝚝𝚑𝚜 𝚊𝚛𝚎 𝚊𝚝𝚝𝚛𝚒𝚋𝚞𝚝𝚎𝚍 𝚝𝚘 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚝𝚑𝚊𝚝 𝚠𝚎𝚛𝚎 𝚑𝚊𝚛𝚟𝚎𝚜𝚝𝚎𝚍 𝚒𝚗 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊.
𝚃𝚑𝚎 𝚝𝚠𝚘 𝚙𝚎𝚘𝚙𝚕𝚎 𝚊𝚝𝚎 𝚝𝚑𝚎 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚊𝚝 𝚝𝚠𝚘 𝚜𝚎𝚙𝚊𝚛𝚊𝚝𝚎 𝚛𝚎𝚜𝚝𝚊𝚞𝚛𝚊𝚗𝚝𝚜, 𝚘𝚗𝚎 𝚒𝚗 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝚊𝚗𝚍 𝚝𝚑𝚎 𝚘𝚝𝚑𝚎𝚛 𝚒𝚗 𝙵𝚕𝚘𝚛𝚒𝚍𝚊. 𝙾𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚍𝚒𝚍 𝚗𝚘𝚝 𝚙𝚛𝚘𝚟𝚒𝚍𝚎 𝚝𝚑𝚎 𝚗𝚊𝚖𝚎𝚜 𝚘𝚏 𝚝𝚑𝚎 𝚛𝚎𝚜𝚝𝚊𝚞𝚛𝚊𝚗𝚝𝚜.
𝚂𝚝𝚊𝚝𝚎 𝚘𝚏𝚏𝚒𝚌𝚒𝚊𝚕𝚜 𝚒𝚗 𝙻𝚘𝚞𝚒𝚜𝚒𝚊𝚗𝚊 𝚜𝚊𝚒𝚍 𝚝𝚑𝚎𝚛𝚎 𝚊𝚛𝚎 𝚗𝚘𝚠 𝚜𝚒𝚡 𝚝𝚘𝚝𝚊𝚕 𝚍𝚎𝚊𝚝𝚑𝚜 𝚏𝚛𝚘𝚖 𝚅𝚒𝚋𝚛𝚒𝚘 𝚟𝚞𝚕𝚗𝚒𝚏𝚒𝚌𝚞𝚜 𝚕𝚒𝚗𝚔𝚎𝚍 𝚝𝚘 𝚝𝚑𝚎 𝚜𝚝𝚊𝚝𝚎. 𝙸𝚝 𝚒𝚜 𝚞𝚗𝚌𝚕𝚎𝚊𝚛 𝚒𝚏 𝚝𝚑𝚎 𝚘𝚝𝚑𝚎𝚛 𝚏𝚘𝚞𝚛 𝚍𝚎𝚊𝚝𝚑𝚜 𝚠𝚎𝚛𝚎 𝚌𝚊𝚞𝚜𝚎𝚍 𝚋𝚢 𝚎𝚊𝚝𝚒𝚗𝚐 𝚘𝚢𝚜𝚝𝚎𝚛𝚜 𝚘𝚛 𝚏𝚛𝚘𝚖 𝚘𝚙𝚎𝚗 𝚠𝚘𝚞𝚗𝚍𝚜 𝚒𝚗 𝚠𝚊𝚝𝚎𝚛.
𝙲𝚊𝚜𝚎𝚜 𝚘𝚏 𝚝𝚑𝚎 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊 𝚊𝚛𝚎 𝚘𝚗 𝚝𝚑𝚎 𝚛𝚒𝚜𝚎.
𝙰𝚌𝚌𝚘𝚛𝚍𝚒𝚗𝚐 𝚝𝚘 𝚝𝚑𝚎 𝙲𝙳𝙲, 𝚝𝚑𝚎 𝚙𝚘𝚝𝚎𝚗𝚝𝚒𝚊𝚕𝚕𝚢 𝚍𝚎𝚊𝚍𝚕𝚢 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊 𝚝𝚑𝚛𝚒𝚟𝚎 𝚒𝚗 𝚌𝚘𝚊𝚜𝚝𝚊𝚕 𝚠𝚊𝚝𝚎𝚛𝚜 𝚍𝚞𝚛𝚒𝚗𝚐 𝚠𝚊𝚛𝚖𝚎𝚛 𝚖𝚘𝚗𝚝𝚑𝚜, 𝚎𝚜𝚙𝚎𝚌𝚒𝚊𝚕𝚕𝚢 𝚒𝚗 𝚋𝚛𝚊𝚌𝚔𝚒𝚜𝚑 𝚠𝚊𝚝𝚎𝚛𝚜, 𝚠𝚑𝚎𝚛𝚎 𝚏𝚛𝚎𝚜𝚑 𝚠𝚊𝚝𝚎𝚛 𝚖𝚎𝚎𝚝𝚜 𝚝𝚑𝚎 𝚜𝚎𝚊.
𝙲𝚊𝚜𝚎𝚜 𝚘𝚏 𝚏𝚕𝚎𝚜𝚑-𝚎𝚊𝚝𝚒𝚗𝚐 𝚋𝚊𝚌𝚝𝚎𝚛𝚒𝚊 𝚠𝚎𝚛𝚎 𝚘𝚗𝚌𝚎 𝚕𝚊𝚛𝚐𝚎𝚕𝚢 𝚌𝚘𝚗𝚏𝚒𝚗𝚎𝚍 𝚝𝚘 𝚝𝚑𝚎 𝙶𝚞𝚕𝚏 𝙲𝚘𝚊𝚜𝚝, 𝚋𝚞𝚝 𝚝𝚑𝚎 𝙲𝙳𝙲 𝚜𝚊𝚒𝚍 𝚌𝚊𝚜𝚎𝚜 𝚏𝚛𝚘𝚖 𝟷𝟿𝟾𝟾 𝚝𝚘 𝟸0𝟷𝟾 𝚜𝚞𝚛𝚐𝚎𝚍 𝚊𝚕𝚘𝚗𝚐 𝚝𝚑𝚎 𝙴𝚊𝚜𝚝 𝙲𝚘𝚊𝚜𝚝 𝚠𝚒𝚝𝚑 𝚊𝚗 𝟾00% 𝚒𝚗𝚌𝚛𝚎𝚊𝚜𝚎.
𝚃𝚑𝚎 𝚛𝚒𝚜𝚔 𝚏𝚘𝚛 𝚅𝚒𝚋𝚛𝚒𝚘 𝚒𝚗𝚏𝚎𝚌𝚝𝚒𝚘𝚗𝚜 𝚑𝚊𝚜 𝚊𝚕𝚜𝚘 𝚜𝚙𝚛𝚎𝚊𝚍 𝚏𝚊𝚛𝚝𝚑𝚎𝚛 𝚗𝚘𝚛𝚝𝚑 𝚊𝚜 𝚠𝚊𝚝𝚎𝚛 𝚝𝚎𝚖𝚙𝚎𝚛𝚊𝚝𝚞𝚛𝚎𝚜 𝚑𝚊𝚟𝚎 𝚒𝚗𝚌𝚛𝚎𝚊𝚜𝚎𝚍 𝚍𝚞𝚎 𝚝𝚘 𝚌𝚕𝚒𝚖𝚊𝚝𝚎 𝚌𝚑𝚊𝚗𝚐𝚎.
𝙰𝚌𝚌𝚘𝚛𝚍𝚒𝚗𝚐 𝚝𝚘 𝚝𝚑𝚎 𝙲𝙳𝙲, 𝚊𝚋𝚘𝚞𝚝 𝟷 𝚒𝚗 𝟻 𝚙𝚎𝚘𝚙𝚕𝚎 𝚠𝚒𝚝𝚑 𝚝𝚑𝚎 𝚒𝚗𝚏𝚎𝚌𝚝𝚒𝚘𝚗 𝚍𝚒𝚎.
Contaminated oysters spread fatal flesh-eating bacteria in two states
Two latest deaths were traced back to Louisiana-harvested oysters
Two people have died after eating oysters contaminated with flesh-eating bacteria, health officials confirmed, and others have been infected.
Both of the fatal cases were traced to Louisiana-harvested oysters that ended up on plates in restaurants in Louisiana and Florida.
The bacterium, Vibrio vulnificus, has now been linked to six deaths in Louisiana and five deaths in Florida, according to the states' health departments.
The rising number of outbreaks prompted the Louisiana Department of Health to issue a statement July 31, urging residents to take precautions against vibriosis, the infection caused by Vibrio vulnificus.
Vibrio vulnificus is part of a wider group of Vibrio bacteria, which are found in coastal waters, the Centers for Disease Control and Prevention states.

Most people get vibriosis by eating raw or undercooked shellfish, particularly oysters, according to the CDC. In some cases, it can also enter open wounds while people are swimming. (iStock)
Vibrio has the potential to cause severe infections, according to Dr. Andrew Handel, pediatric infectious diseases specialist at Stony Brook Children's Hospital in New York.
These include invasive soft tissue infections (sometimes called "necrotizing fasciitis" or "flesh-eating bacteria") and bloodstream infections.
Most people get vibriosis by eating raw or undercooked shellfish, particularly oysters, according to the CDC.
In some cases, it can also enter open wounds while people are swimming.

People who have eaten contaminated shellfish will have severe vomiting and diarrhea, which can lead to dehydration, health officials caution. (iStock)
Prior to this incident, health officials reported 17 cases of Vibrio vulnificus among Louisiana residents in 2025. All patients were hospitalized, and four of those illnesses resulted in death.
Over the previous 10 years, an average of seven Vibrio vulnificus cases and one death were reported each year in Louisiana.
"It’s just prolific right now," Jennifer Armentor, the molluscan shellfish program administrator at the Louisiana Department of Health, told the Louisiana Oyster Task Force Tuesday at the New Orleans Lakefront Airport.
Symptoms to watch for
Vibriosis symptoms depend on the type of infection, according to Handel.
"The symptoms of skin infections can progress quickly and become life-threatening in a short time," he previously told Fox News Digital. "Thankfully, those infections are rare."
"If you do eat shellfish, make sure it has not been sitting out for a long time and comes from a hygienic source."
People who have eaten contaminated shellfish will have severe vomiting and diarrhea, which can lead to dehydration, the doctor warned.
While healthy people generally experience only mild symptoms, those who are immunocompromised or have chronic liver disease can face serious health risks.

A bacterial infection is diagnosed by testing cultures obtained from stool, wounds or blood. (iStock)
If Vibrio vulnificus enters the bloodstream, it can cause severe illness marked by fever, chills, septic shock and blistering skin lesions, according to Florida Health. About half of these bloodstream infections are fatal.
Some severe cases can cause necrotizing fasciitis, which is when the flesh around an open wound dies, the CDC cautions.
Diagnosis and treatment
The bacterial infection is diagnosed by testing cultures obtained from stool, wounds or blood, according to health officials.
For mild infections, the CDC recommends increasing fluid intake to prevent dehydration.

About one in five people will die from a vibriosis infection, sometimes within a day or two of the illness. (iStock)
Those with severe or prolonged infections should receive antibiotics to improve survival rates. For people with infected wounds, surgery may be necessary to remove dead tissue.
About one in five people will die from the infection, sometimes within a day or two of the illness, the CDC states.
"To prevent Vibrio food poisoning, avoid eating raw shellfish, especially if you are immunocompromised or have chronic liver disease," Handel advised.
The doctor noted that Vibrio infections are rare and "should not be a major cause of alarm."
"If you do eat shellfish, make sure it has not been sitting out for a long time and comes from a hygienic source."
Fox News Digital's Melissa Rudy contributed reporting.
Khloe Quill is a lifestyle production assistant with Fox News Digital. She and the lifestyle team cover a range of story topics including food and drink, travel, and health.
How to Eat Oysters Safely: Important Tips to Protect Your Health
Oysters are a popular seafood enjoyed around the world for their unique taste and nutritional value. However, eating oysters improperly — especially raw oysters — can pose serious health risks. Health experts emphasize that following proper safety guidelines is essential to avoid foodborne illnesses.
Understand the Risks of Raw Oysters
Raw or undercooked oysters may contain harmful bacteria such as Vibrio, which naturally live in warm coastal waters. These bacteria are invisible, odorless, and cannot be detected by taste.
In some cases, infections can become severe and even life-threatening, particularly for people with weakened immune systems.
Choose Oysters from Reliable Sources
Buy oysters only from licensed and reputable suppliers
Avoid oysters harvested from unregulated or unknown waters
Check that oysters are properly refrigerated and stored
Restaurants and seafood markets should follow strict food safety regulations to reduce contamination risks.
Cook Oysters Thoroughly
Cooking is the most effective way to kill harmful bacteria. Health authorities recommend:
Boiling oysters until shells open and continuing to boil for at least 3–5 minutes
Steaming oysters for 4–9 minutes
Frying, baking, or grilling oysters until the flesh is firm and fully cooked
Avoid eating oysters that do not open during cooking.
Be Extra Careful if You Are High-Risk
The following groups should avoid raw oysters completely:
People with liver disease
Individuals with weakened immune systems
Pregnant women
Older adults
For these individuals, even a small amount of contaminated seafood can cause serious illness.
Practice Good Food Hygiene
Wash hands thoroughly before and after handling raw seafood
Keep raw oysters separate from other foods
Clean knives, cutting boards, and surfaces after use
Proper hygiene helps prevent cross-contamination.
Know the Warning Signs
Seek medical attention immediately if you experience symptoms such as:
Fever
Vomiting or diarrhea
Severe stomach pain
Skin wounds that become red, swollen, or painful after seawater exposure
Early treatment can be life-saving.
May you like
Conclusion
Oysters can be enjoyed safely when handled and prepared correctly. Choosing reliable sources, cooking oysters thoroughly, and understanding personal health risks are key steps to protecting yourself and your family.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice.